Cardiology
European Society of Cardiology (ESC) Congress 2019
THEMIS-PCI: Potent Dual Antiplatelet Regimen Found Beneficial in Diabetic Patients with CAD and History of PCI
Paris – For patients with type 2 diabetes mellitus (T2DM) and coronary artery disease (CAD) who have had a prior percutaneous coronary intervention (PCI), the new antiplatelet substudy, THEMIS-PCI, is the first in this specific patient population. In the main THEMIS trial, 19,220 T2DM patients ≥50 years with stable CAD were randomized to dual antiplatelet therapy (DAPT) or aspirin alone. Although the dual antiplatelet regimen was associated with a reduced risk of major adverse cardiovascular events (MACE) in all participants, the net clinical benefit, after accounting for increased risk of bleeding, was only considered favorable in the THEMIS-PCI substudy.
The main trial, called THEMIS which is the largest cardiovascular (CV) outcomes trial in diabetic patients, and the substudy, called THEMIS-PCI, were presented in sequence at the 2019 ESC meeting. The 11,154 PCI patients in THEMIS-PCI, representing 58% of the THEMIS trial population, were a prespecified subgroup. All patients were randomized to the P2Y12 inhibitor ticagrelor or placebo, each administered with aspirin. The net clinical benefit, calculated for both groups, was most apparent for the PCI patients.
The data suggest that DAPT is a new option for this selected patient population.
While DAPT and MACE benefit is established in patients with T2DM and a history of myocardial infarction (MI), THEMIS-PCI is the first time it has been studied in a diabetic patient population with CAD, but no history of MI. “The data suggest that long-term DAPT with ticagrelor is a new option for this selected patient population,” according to Dr. P. Gabriel Steg, Director of the Coronary Care Unit, Hôpital Bichat, Université de Paris – Diderot, France. He presented the data from the PCI substudy immediately after the full THEMIS dataset was presented by Dr. Deepak L. Bhatt, Brigham and Women’s Hospital, Harvard Medical School, Boston, Massachusetts.
Benefit Narrows in Absence of PCI History
In THEMIS overall, the risk-to-benefit advantage of the DAPT was narrow, leading Dr. Bhatt to conclude that this strategy “may only be beneficial in selected patients at low risk of bleeding but with a high risk of ischemic events.”
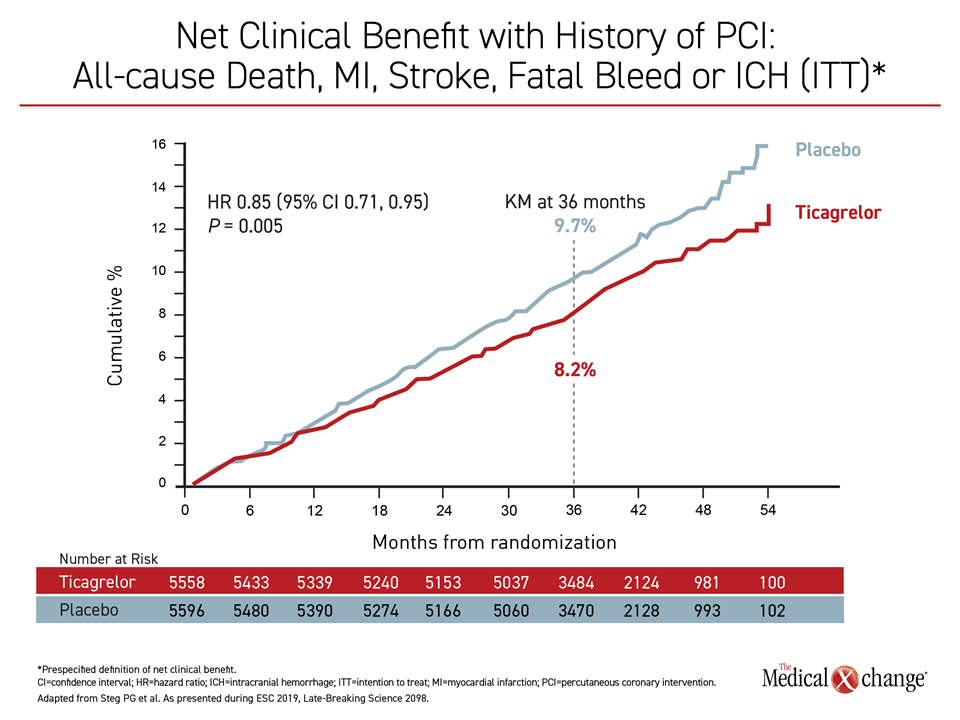
In THEMIS-PCI, DAPT was associated with a statistically significant 15% (HR 0.85; P=0.005) reduction in irreversible harm events, which includes MACE and bleeding events, according to Dr. Steg (Figure 1).
The phase 3 THEMIS trial was designed to evaluate whether DAPT with ticagrelor, a reversible P2Y12 inhibitor, and aspirin could safely reduce the risk of CV events in T2DM patients with stable CAD but no prior history of MI or stroke. This group remains at high risk of CV events despite therapy of aspirin alone. More effective than aspirin or the P2Y12 inhibitor clopidogrel, ticagrelor is already part of standard DAPT for other high-risk indications, such as the treatment of acute coronary syndromes.
THEMIS and THEMIS-PCI Data Published
In THEMIS, which was published simultaneously with a presentation at ESC (Steg PG et al. N Engl J Med. 2019; Sept 1 [epub ahead of print]), the nearly 20,000 T2DM patients with stable CAD were enrolled at centers worldwide. After a median 39.9 months of follow-up, the primary composite efficacy endpoint of CV death, MI, or stroke was reached by 7.7% of those randomized to ticagrelor plus aspirin and 8.5% of those on aspirin plus placebo, providing a 10% (HR 0.90; P=0.04) reduction favoring DAPT.
However, rates of major bleeding were higher in the DAPT group on several measures, including the TIMI (Thrombolysis in MI) criteria (HR 2.32; P<0.001). When the incidence of irreversible harm was calculated, the 7% relative benefit for DAPT (HR 0.93; 95% CI 0.86-1.02) was no longer statistically significant. This was not the case in the THEMIS-PCI subgroup evaluation, which was also published simultaneously with its presentation at ESC (Bhatt DL et al. Lancet 2019; Sept 1 [epub ahead of print]).
Better Benefit-to-Risk in PCI Patients
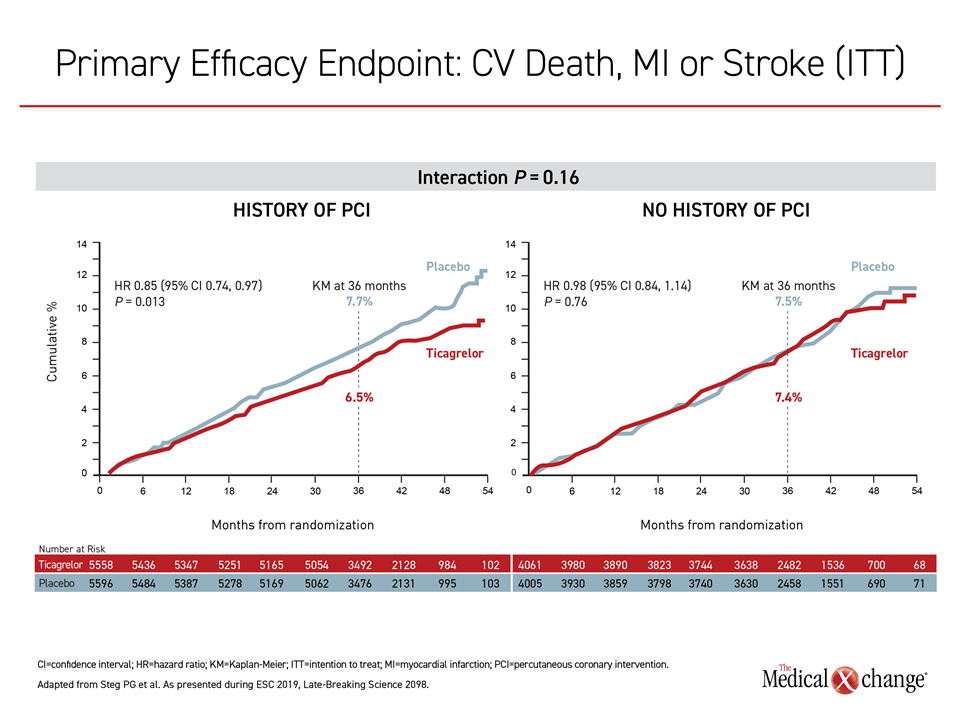
Comparing the groups side by side, Dr. Steg associated DAPT with a 15% (HR 0.85; P=0.013) relative improvement for the primary efficacy endpoint relative to placebo for those with a history of PCI but only a slight and non-significant benefit in those without a history of PCI (Figure 2). The differences in bleeding were not significantly lower in the PCI group, but many of the bleeding outcomes were numerically lower, including TIMI major bleeding (2.0% vs. 2.4%) fatal bleeding (0.1% vs. 0.3%) and intracranial bleeding (0.6% vs. 0.9%).
These differences explain the net 15% relative benefit on the endpoint of irreversible harm favoring ticagrelor-based DAPT in the T2DM patients with a history of PCI, according to Dr. Steg. As seen in Figure 1, the curves favoring DAPT continued to separate after the end of the median follow-up, and this separation has persisted for the duration of follow-up so far. Both he and Dr. Bhatt said that the advantage of the ticagrelor-based DAPT is clinically meaningful. “We have data extending beyond five years suggesting that the benefit of the DAPT [in T2DM patients with history of PCI] extends at least over this period,” Dr. Bhatt reported.
In patients at risk of new or recurrent MACE, antiplatelet treatments, like anticoagulants, reduce ischemic events at a cost of increased bleeding. The history of trials with these agents has revolved around identifying a favorable trade-off. If methods to identify the high risk of ischemic events but a low risk of bleeding improve, there will be new opportunities to target DAPT treatment in patients with T2DM and CAD, but Dr. Bhatt and Dr. Steg agreed that the THEMIS data demonstrated net benefit in the PCI subgroup.
Conclusion
In T2DM patients with a history of CAD, a multinational trial was unable to demonstrate a compelling advantage among unselected patients for a ticagrelor-based DAPT due to an increased risk of bleeding. However, in a subgroup of stable CAD patients with T2DM and a history of PCI, which represented 58% of the THEMIS trial population, the relative efficacy advantage was increased, providing a net reduction in irreversible events favoring DAPT. These data identify a new approach to risk management in this population.